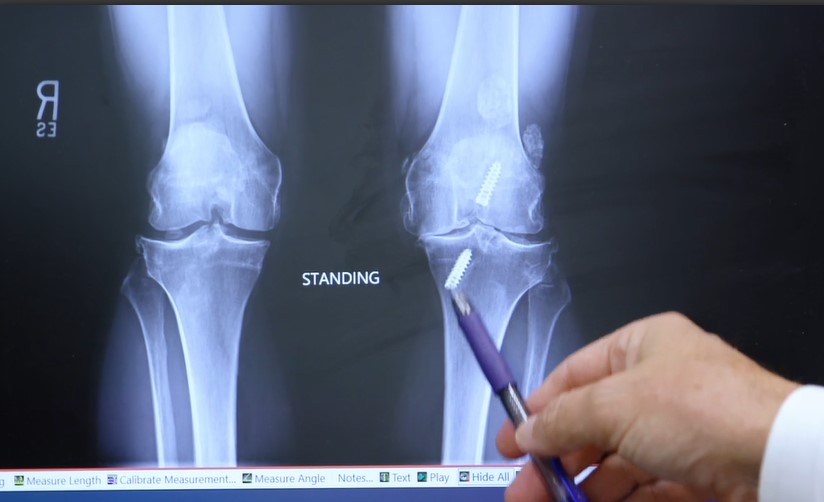
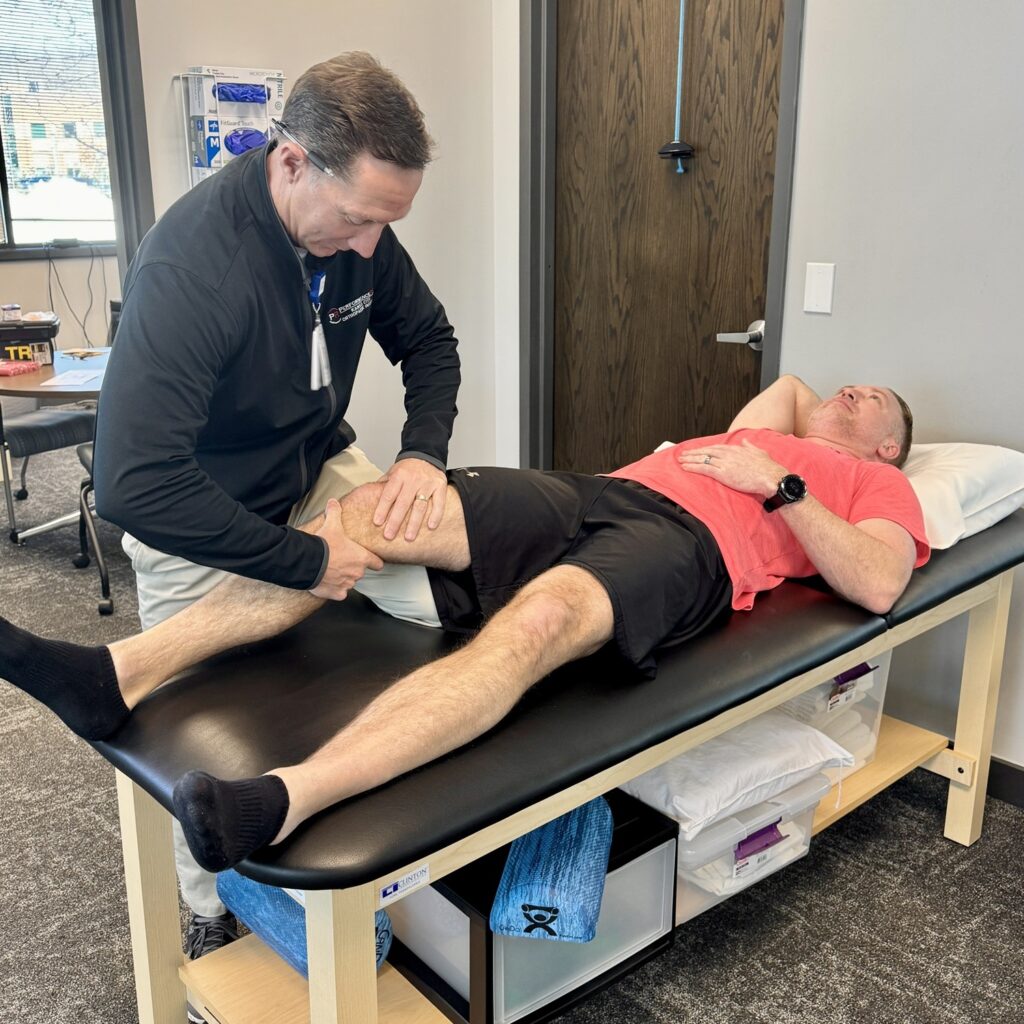
An injury has a way of changing everything including how you move, how you work, and how confident you feel in your day-to-day life. Whether it happens suddenly or develops over time, the loss of independence can be just as challenging as the physical pain itself.
At Kansas City Orthopaedic Institute (KCOI), we help patients move forward stronger, safer, and more confident than before. As a physician-owned orthopedic hospital, we are structured differently, and that difference shows how patients experience care from the moment they arrive.
Care Designed Around the Patient
Because KCOI is physician-owned, care decisions are led by the people who know orthopedic conditions best: orthopedic specialists themselves. That structure allows for faster collaboration, more personalized treatment plans, and a level of focus that is hard to find in traditional hospital systems.
Instead of navigating multiple facilities, patients benefit from a connected care team including surgeons, a 1:2 ratio for nurses to patients, therapists, and other support staff, working together in one environment built specifically for orthopedic care.
As Julie Murphy, Hospital Admissions Rep at KCOI said, “I work at KCOI because I love taking care of the patients and watching everyone else take care of the patients in an excellent way.”
You can explore our full team of board-certified, fellowship trained specialists on our Providers’ page, where expertise spans joint replacement, sports medicine, spine, foot and ankle, hand, and wrist, and more.
When Injuries Happen, Speed Matters
Orthopedic injuries don’t wait for a convenient time. A fall, a sports injury, or a sudden twist can instantly change a normal day into a stressful one. That’s why immediate access to specialized care matters is important.
For patients searching for orthopedic urgent care near me, KCOI offers Ortho Urgent Care seven days a week that is staffed by providers who focus exclusively on musculoskeletal injuries. Unlike a general emergency room, our urgent care is designed specifically for bone, joint, and muscle injuries. We treat every day orthopedic injuries as well as sports injuries for competitive and recreational athletes, including:
- Broken bones (fractures)
- Sprains, strains, and other muscle or tendon injuries
- Torn ACL, torn MCL and other ligament injuries
- Muscle contusions and minor lacerations.
Our Ortho Urgent Care provides fast access to orthopedic experts who can diagnose injuries accurately and create a clear path forward—often preventing delays that can slow recovery.
A Seamless Path from Diagnosis to Recovery
One of the biggest challenges patients face after an injury or surgery is fragmentation or being passed from one provider to another with little coordination. At KCOI, care is intentionally integrated.
From advanced imaging and surgical suites to inpatient care and rehabilitation, services are designed to work together. Surgeons communicate directly with therapists. Nurses coordinate closely with care teams. Patients know what comes next—and who to call with questions.
Rehabilitation That Builds Strength and Confidence
Recovery is not just about healing tissue. It’s about rebuilding trust in your body.
Through KCOI’s rehabilitation services, patients receive personalized physical and occupational therapy focused on real-life goals including walking without pain, returning to work, getting back on the field, or simply moving without hesitation.
Therapists work closely with physicians to adjust treatment plans as progress is made, helping patients regain both mobility and independence.
Being a physician-owned orthopedic hospital means KCOI is built around outcomes—not volume. Our teams are aligned around quality, efficiency, and patient experience, which translates to:
- Shorter wait times
- Specialized orthopedic nursing care with one registered nurse for every two patients!
- Streamlined transitions from surgery to rehab
- Consistently high patient satisfaction
This focus allows patients to feel supported at every stage of their journey, rather than lost in a complex system.
As the parent(s) of 3 daughters in medicine: A M.D, Pharm-D, BSN R.N. & a S.I.L. Pulmonologist M.D. (PCC), & since 2010 having had 3 total joint replacements @ KCOI, (2 knees & a shoulder), I can attest as to the professionalism of the Orthopedic Doctors, their Physician Assistants, the R.N. Nurses on the floor with a 1 to 2 ratio, (1 R.N. for every 2 patients)…the Medical Assistants, Schedulers & the Physical Therapists of Performance Rehab.
The professionalism & quality of care are reasons why KCOI is rated in the top 2% of the hospitals in the NATION and ranked the number ONE joint replacement hospital in the state of Kansas.
From the 30 Physicians of the physician-owned hospital, to the security guard who assists you into your car at dismissal, ALL the employees are extremely kind & interested in your complete recovery. The morale, esprit de corp & low to no staff turnover at KCOI are virtually unheard of in today’s medical hospitals, and bear witness to the character and professionalism of all of the employees at KCOI.”
– Vincent W.
Helping Patients Return to What Matters Most
Success is not measured by procedures alone; it is measured by what patients are able to do again. Return to work. Return to sports. Return to daily routines without pain or fear.
Whether care begins with urgent treatment, a physician visit, or surgery, KCOI’s role is to guide patients from injury to independence with clarity, expertise, and compassion.
If you are looking for orthopedic urgent care near me or exploring treatment options at a specialized orthopedic facility, learn more about our approach at kcoi.com or contact our team directly.